There is a kind of exhaustion that never appears in a hospital file.
It is the exhaustion of a mother who has spent another night listening to her child cry through a pain crisis.
It is the exhaustion of a father who has borrowed bus fare again, missed work again, and sat on another hospital bench praying that this time the blood will be available, the doctors will move quickly, and the child will come through.
Sickle cell disease does not only attack the body.
It can quietly drain a family’s money, sleep, strength, and hope.
That is why the new Spectra Optia Apheresis Machine at Jaramogi Oginga Odinga Teaching and Referral Hospital, or JOOTRH, matters so deeply. JOOTRH says the machine gives sickle cell patients access to apheresis treatment “without delay or uncertainty,” and says it is the first public hospital in Kenya to own the technology.
For many families, sickle cell is not one dramatic emergency. It is repeated disruption. A child misses school. A parent misses work. Rent competes with transport. Food competes with treatment. Then comes another crisis, another admission, another search for blood, another round of fear.
Reporting on the Kisumu rollout says the machine is being used for red blood cell exchange, a procedure that is critical in managing severe sickle cell complications such as stroke and acute chest syndrome.
What the machine actually does
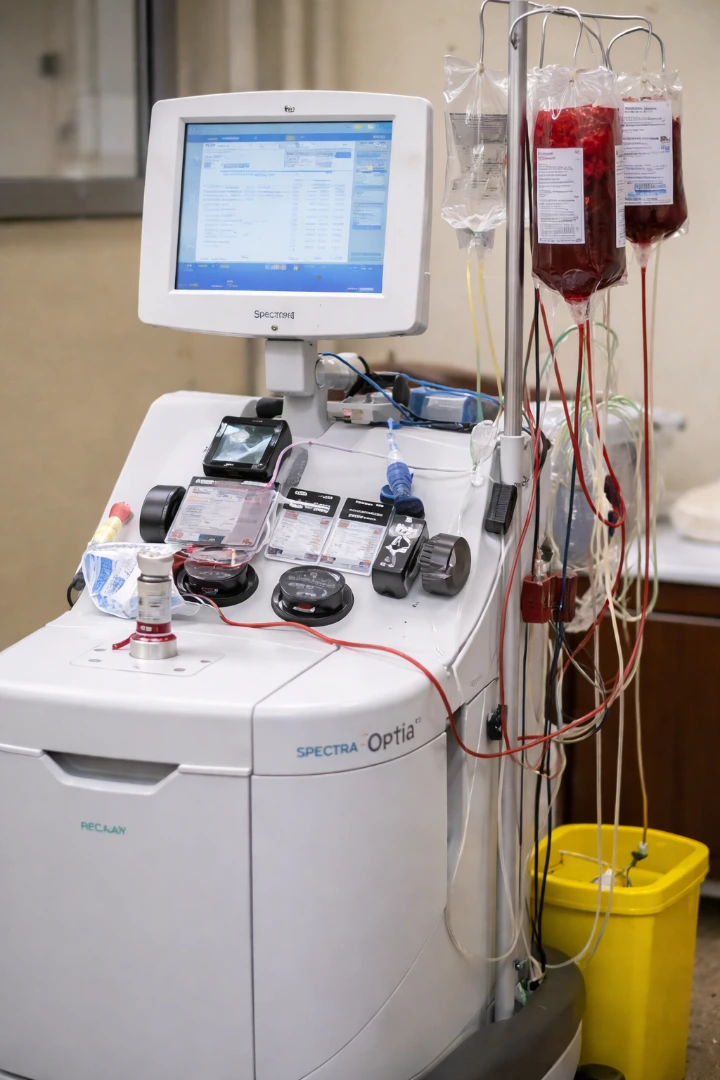
The machine performs automated red blood cell exchange.
In simple terms, blood is taken from the patient, the machine separates out the red blood cells, removes many of the damaged or sickled cells, and replaces them with healthy donor red blood cells while returning the rest of the blood components.
JOOTRH says the system removes damaged red blood cells and replaces them with healthy ones, while its January special edition explains that the process uses centrifugation to separate blood components before replacing the sickled cells.
To a parent, that technical process means something very human: fewer sickled cells blocking blood vessels, less risk of catastrophic complications, and a better chance of preventing the kind of crisis that turns a normal day into panic.
JOOTRH’s own reporting around its first automated exchange described the treatment as a milestone that can reduce painful crises, help prevent strokes, and improve quality of life.
How long treatment takes
The procedure itself is not endless, though the hospital day can feel long. JOOTRH has described the red cell exchange as taking about two hours. Patient guidance from University College London Hospitals says the procedure usually takes about two hours as well, though the full visit can take longer because of preparation, line placement, blood checks, and monitoring.
How often a child might need it
This depends on why the child is getting exchange treatment. There is no single schedule for every patient. JOOTRH said in 2025 that the procedure may be repeated two to three times a year in some cases. But major sickle cell exchange programs also note that patients on a regular prevention program may need exchanges every four to eight weeks, with many receiving them roughly every five weeks. That means one child may need it occasionally, while another may need it on a near-monthly schedule to reduce stroke risk or control severe disease.
That matters emotionally as much as clinically. For a parent, a one-off treatment is one kind of burden.
A recurring program every month or so is another. It means planning transport, arranging school, finding time away from work, and preparing yourself emotionally for a hospital rhythm that keeps returning.
But when the service is available nearby and more reliably, that rhythm becomes less chaotic.
JOOTRH says the permanent machine now offers uninterrupted and sustainable access for patients who had previously faced long waiting periods.
How much it costs
This is the part many families want answered first, and the honest answer is that the exact JOOTRH patient charge is not clearly published in the public sources .
What is clear is that the treatment has publicly been described as expensive, and the need for subsidy or broader coverage has been raised in public discussion around sickle cell care in Kenya.
But sometimes Cost may not be a big factor,when it comes to human life -
And this is where the emotional truth of the story sits. The pain is not only watching your child suffer. It is the arithmetic of chronic illness. School fees or treatment. Rent or transport. Time at work or time in the ward. Blood donor calls or meals at home. A machine like this does not erase sickle cell disease, but it can remove part of the uncertainty that makes every episode heavier.
The stress this machine may lift
The biggest relief may not be visible in the machine’s screen.
It may show up in a mother sleeping a little easier because she knows the service exists closer to home.
It may show up in a father missing fewer days of work because the procedure is faster and more predictable. NICE’s assessment of Spectra Optia found evidence of shorter procedure times than manual exchange and longer average intervals between procedures in the evidence it reviewed. For families, that can mean less time in crisis mode and more time living ordinary life.
It may also mean fewer terrifying moments around severe complications. The machine is specifically linked to managing or preventing stroke and acute chest syndrome, two of the most frightening complications in sickle cell disease. For a parent, even the possibility of lowering that risk can feel like light returning after a long period of fear.
Why this story is bigger than one machine
This is not only a story about equipment. It is a story about access. JOOTRH is not just using the machine; it is also building broader sickle cell leadership. The hospital has described its work as part of a wider push to transform sickle cell and hemophilia care in western Kenya, and recent reporting says a JOOTRH radiologist won an international grant to lead a stroke-prevention study in children living with sickle cell disease. That suggests the hospital is building not just a service, but a center of seriousness around this condition.
For the parent of a child with sickle cell disease, this machine is not just metal, tubing, and screens.
For the parent of a child with sickle cell disease, this machine is not just metal, tubing, and screens.

It is time saved. Panic interrupted. Pain reduced. It is one less desperate search for help. One less exhausting journey into uncertainty. One more reason to believe that advanced care does not always have to be far away.
And for families who have carried this burden for years, that kind of hope is not small at all.
Written by :Justina Mwongeli